Shoulder instability develops in two different ways: traumatic onset (associated with sudden injury) or atraumatic onset (apart from sudden injury). Understanding the differences is important in choosing the best treatment. Typically, patients with early atraumatic instability will experience generalised looseness (sagging) in the joints that eventually lead to shoulder instability. In contrast, traumatic instability begins when the injury results in repeated (recurring) shoulder dislocations.
When the shoulder is unstable, the patient can feel the shoulder slipping from the socket and weak. These instances of instability are not always painful.
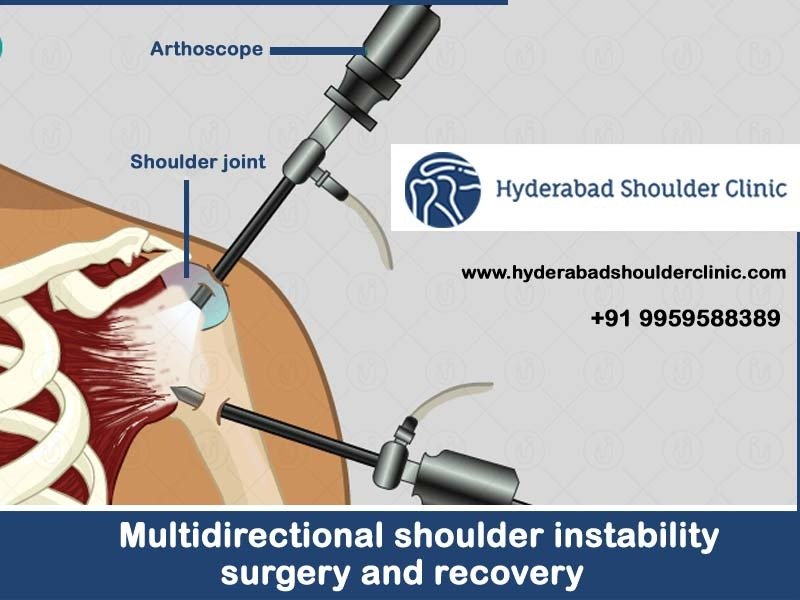
This article provided by Dr Chandra Shekar gives information about Multidirectional shoulder instability surgery recovery. Before that, let us see what shoulder joint is and Multidirectional shoulder instability, and surgical procedure.
What is the shoulder joint?

The shoulder joint is a complex joint structured to allow for more movement than any other joint in the body. This joint’s range of motion is usually well controlled and stable, but it can be too flexible in some people, which can lead to shoulder dislocation. People whose shoulders are not as tight as they should, have shoulder instability.
Shoulder instability is a condition where the ball can pop out of the socket at the ball shoulder joint and socket. Sometimes the ball is partially out of the socket – a condition described as subluxation of the shoulder. But when the ball does come out of the socket, it’s a shoulder dislocation.
There are two types of shoulder instability:

Traumatic instability: Traumatic shoulder instability occurs due to acute shoulder injuries such as falls or sports injuries. The shoulder is forcibly pulled out of the socket and often has to be relocated using special manoeuvres and may require anaesthesia. Traumatic dislocations can damage the ligaments that hold the ball in the socket, making the shoulder more prone to dislocations in the future.
Multidirectional instability: Multidirectional instability (MDI) occurs when the shoulder joint loosens in the socket. This is not necessarily a traumatic event that causes instability; conversely, the shoulder tends to shift excessively, resulting in pain and reduced joint function. People with symptoms of multidirectional instability often complain of tension or displacement of the shoulders with overhead movements.
Atraumatic shoulder instability, also known as multidirectional instability (MDI), occurs in patients who have more relaxation of the ligaments surrounding the glenohumeral shoulder joint. This looseness can be a natural state (available from birth) or a state that develops over time.
How could it be?

The shoulder is the most flexible joint in the human body, with a complex arrangement of structures that work together to provide the movement needed in everyday life. There are four bones and soft tissues (ligaments, tendons, and muscles) that cause shoulder movement. They interact to keep joints in place when moving through extreme areas. Each of these structures makes an important contribution to shoulder movement and stability. Certain work activities or sports can place heavy loads on the shoulders and cause injury if the limits of movement and overload of the individual structure are exceeded.
Some people naturally have loose connections, which can cause them to experience instability. Shoulder instability can also occur in people who regularly perform shoulder movements that stretch the joint capsule. Gymnasts, ball pitchers, volleyball players and swimmers are at greater risk of shoulder instability. Sometimes a sudden injury makes symptoms worse. In case of multidirectional instability, the arm is loosened by moving in several directions. This differs from patients with instability after shoulder sprains that occur as a result of traumatic injuries. These people are usually one-way careless.
How is it treated?

Usually, non-surgical options are the first goal.
- Rest – Avoid painful activities or activities that put pressure on the joints
- Ice – Helps control pain, especially after exercise.
- Medications – Non-steroidal anti-inflammatory drugs can be used to treat pain, such as Ibuprofen
- Physiotherapy – Most MDI patients can be treated with a physical therapy program that focuses on muscle rehabilitation. This involves strengthening the rotator cuff muscles and the muscles around the shoulder blades, which add dynamic stability to the joint. To achieve these results, the patient must follow the rehabilitation program carefully for a minimum of 6 months.
Does a patient need an operation?
If non-surgical options fail to relieve MDI symptoms and daily activities are disturbed, surgery may be considered. One can do this arthroscopically – a small camera is inserted through a small incision in the shoulder, or an open procedure may be required. Both procedures reduce the size of the joint capsule to limit movement in the glenohumeral joint. Physiotherapy is required after surgery to restore strength and freedom of movement.
Surgery
MDI’s surgical procedure is considered in patients who have persistent symptoms of shoulder instability despite non-surgical treatment. Often, the ligaments that surround the shoulder are tightened during surgery. This can be done by minimally invasive arthroscopic surgery or by standard surgical incisions.
The best surgery for multidirectional instability is capsule replacement. This is a procedure used to tighten the shoulder capsule. Closing the rotator cuff is the process of closing the gap between the two muscles on the rotator cuff.
Thermal shrinkage procedures have very poor results and often require additional surgical treatment. If you have thermal contractions, surgery may be needed if symptoms recur.
Rehabilitation after surgery for multidirectional instability takes several months. After surgery, the shoulder is immobilised first so that the tight tissue can heal. Then a movement to restore mobility begins, followed by strengthening exercises. Most athletes can resume full activity within six months.
Traditional approach
Traditional MDI surgery is designed to shrink the joint capsule and reduce glenohumeral movement. This open surgical procedure is called extensive inferior capsular release and imbrication.
- The bottom of the joint capsule is cut and stacked to tighten the ligaments and make the capsule smaller.
- During this process, the subscapularis muscle is removed so that the surgeon can access the joint capsule. It will be placed again at the end of the operation.
- This procedure’s success rate is about 75% in a carefully selected group of people (those who have been identified as good surgical candidates). As this procedure can result in a significant loss of motion, the athlete may not return to racing after surgery.
Arthroscopic Technique

Recently, arthroscopic techniques have been developed to correct multidirectional instability.
- Capsule lining (fold and suture technique) uses arthroscopic sutures to reduce the joint capsule’s size.
- Thermal capsulorrhaphy is a technique that uses heat energy to shrink capsules. This method is appreciated and looks promising because it is less invasive and can reduce loss of motion.
Multidirectional shoulder instability surgery recovery
After operation:

Recovery from an atraumatic shoulder sprain depends on how well your shoulder responds to physical therapy and whether you need surgery. Depending on the severity of the instability, atraumatic shoulder dislocations can be cured within a few weeks with non-surgical treatment.
- Patients usually wear the sling for the first 4 to 6 weeks to protect the repair while it heals.
- During this immobilisation period, elbow and wrist movements are maintained by a series of gentle exercise movements.
- After the initial healing process is complete, the patient begins a very slow and progressive physical therapy rehabilitation program to restore movement and ultimately strengthen the shoulder.
- Patients with open surgery undergo an exercise program to protect the subscapularis muscle from injury. (This muscle has been removed during the procedure to allow surgeons access to the joint capsule and is reconnected at the end of the procedure.)
- Patients undergoing arthroscopy treatment for thermal stabilisation require a longer immobilisation period (often up to 8 weeks) so that scar tissue can replace the heat-treated tissue. This scar tissue is important for this procedure’s success because the heat-treated tissue is at risk of stretching.
- Full participation in sports is usually limited to 9 to 12 months after improvement.
- With repeated use of the shoulder for a long time, atraumatic shoulder dislocation can recur. Therefore, it is important to make shoulder strengthening exercises a priority throughout your sports career.
Conclusion:
Untreated sports injuries can cause additional damage, such as joint sprains and damage to the protective cartilage that protects the bones from wear and tear. Ultimately, this can lead to osteoarthritis, a degenerative disease that causes excruciating pain and stiffness in the affected joint.
Dr Chandra Shekar has extensive experience with sports injuries like Multidirectional shoulder instability offers arthroscopic treatment for all types of musculoskeletal disorders, including rotator cuff and cruciate ligament repair in the shoulder.
For more information about Multidirectional shoulder instability surgery and recovery, contact Dr Chandra Shekar at 91 9959588389.